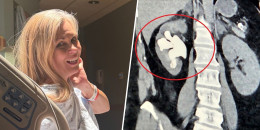
Amanda Peet is opening up about a daunting diagnosis she received while navigating the declining health of both of her parents.
In a new essay for The New Yorker, the actor revealed that she was diagnosed with breast cancer in the fall of 2025, just as her mother and father, who were "long divorced," were both in hospice care.
Peet, 54, explained that doctors have told her she has “dense” breasts many times over the years, requiring extra monitoring. As a result, she'd been seeing a breast surgeon every six months.
When the actor's doctor spotted something concerning on her ultrasound, she performed a biopsy.
"After the procedure, she said that she would walk the sample over to Cedars-Sinai and hand-deliver it to Pathology. That’s when I knew," Peet wrote in the essay, which published March 21.
Dr. Elisa Port, chief of breast surgery for Mount Sinai health system, joined TODAY March 23 to break down Peet’s diagnosis and share what to know about breast cancer in dense breasts. Read on for more details about Peet's diagnosis and breast cancer detection.
How Amanda Peet Learned She Had Breast Cancer
After multiple tests, the “Your Friends & Neighbors” star learned that she had hormone-receptor-positive and HER2-negative breast cancer and would need to undergo a lumpectomy and radiation.
Shortly before she received the official diagnosis, Peet's father died. In her essay, the actor recalled standing in his apartment struggling to balance her grief over his death and the fear related to her impending diagnosis.
"I felt guilty for not crying, but at least I got a reprieve from guessing how much longer I had to live," she wrote.
"As soon as my dad’s corpse was out of sight, I was free to panic about my cancer again," she continued.
Meanwhile, Peet's mother was also in hospice on the opposite side of the country and the actor once again found herself juggling concern for her parent with worry over her own health.
"That Labor Day weekend, though, I found myself unable to visit her cottage at all. I didn’t have the space in my brain for both her disease and mine," she wrote.
When Peet received her diagnosis, she shared the news with her three children, who are 19, 15 and 10.
"My daughters were on the cusp of adulthood. If we were going to remain close, to know each other deeply over the course of a lifetime, we would have to learn how to have difficult conversations," she wrote.
Flash forward to mid-January 2026, and Peet received her first clear scan after treatment. Two weeks later, her mother’s hospice nurse revealed that her mother was close to death.
What to Know About Dense Breasts
Port described "dense breasts" as a "categorization you can only make based on a mammogram."
"You have to have a mammogram to tell you if you have dense breasts because the tissue shows up as whiter and may make it more difficult to see cancer against that background," she said.
According to the Breast Cancer Research Foundation, dense breast tissue occurs in nearly half of all women over the age of 40. It can make breast cancer “harder to detect and more likely to develop.”
Is a Mammogram or Sonogram Better to Detect Breast Cancer?
Oftentimes, doctors order additional testing, such as a sonogram, after detecting something concerning on a mammogram. For this reason, Port said mammograms are an important first step in detecting breast cancer since they pick up 80 - 90% of breast cancers.
"In dense breasts, it could be as low as 60%. So the mammogram is still a very, very important part and it should be the first test. And then we add ultrasounds in someone with dense breasts to try to close the gap on some of the cancers we might be missing through the mammogram," Port said.
What Is Hormone-Receptor-Positive and HER2-Negative Breast Cancer?
There are several types of breast cancer, and in Peet's essay, she shared that hers was hormone-receptor-positive and HER2-negative.
Hormone-receptive-positive breast cancer means the cancer cells have receptors for hormones, which the cells can use for growth, per the Mayo Clinic.
"Most breast cancers have hormone receptors," Mayo Clinic's website reads.
HER2-negative breast cancer means your cancer cells “don’t have excess amounts of HER2 protein," according to the Cleveland Clinic. HER2 stands for human epithelial growth factor-receptor 2.
“With most breast cancers, hormones and/or the HER2 protein fuel cancer growth,” the clinic’s website reads.
Per the Cleveland Clinic, hormone-receptor-positive and HER2-negative breast cancer accounts for “70% of all breast cancers.”
“It involves cancer cells that do have hormone receptors for estrogen (ER+), progesterone (PR+) or both. The hormones fuel tumor growth. But these cancers don’t have high levels of HER2,” the clinic’s website reads.
In Peet's essay, she described receptor status as something that indicates how "tough" the cancer is, comparing it to a spectrum of dogs where “you have poodles on one end and, on the other, pit bulls.”
She wrote she learned of her type when her doctor texted, “All poodle features!”
How Was Amanda Peet's Cancer Treated?
In her essay, Peet wrote that her breast cancer treatment consisted of a lumpectomy and radiation, rather than a double mastectomy or chemotherapy.
A lumpectomy is a surgery that involves removing parts of breast tissue to treat breast cancer, per Mayo Clinic. It's often followed by radiation to lower the risk of recurrence.
When it comes to breast cancer recurrence, Port said the possibility of recurrence "depends on the severity of the case."
"I think it's important to know that with a lumpectomy, which is what the majority of women have for breast cancer, small surgery, the risk of recurrence in that breast is less than 5%. So most women can find that number acceptable, and it's a very low number that they can live with," she said.
"The overall survival rate from breast cancer now for all women overall is about 91%, and so most women will live their lives fully and go on and thrive," she added.